Contents
Skin Conditions and Diabetes
Diabetes can affect many parts of your body, including your skin. Skin conditions in diabetes are often a sign that your blood sugar levels are too high. It could mean-
- You have undiagnosed diabetes or prediabetes
- Your treatment for diabetes needs to be adjusted
Skin Infections In Diabetes
Skin conditions related to diabetes are common. As many as 1 out of 3 people with diabetes will have one. Fortunately, most skin conditions can be successfully treated before they turn into a serious problem. The key is to catch them early. Early diagnosis helps in early treatment.
Before discussing each condition in detail, let me tell you some more common skin problems that a person with diabetes may experience-
Itchy skin
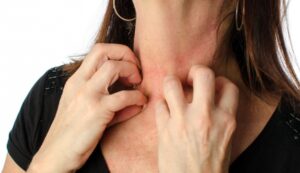
Itching skin, also called pruritus, can have many causes, such as dry skin, poor blood flow, or a yeast infection. When itching is caused by poor blood flow, you’ll likely feel it in your lower legs and feet. And in this case, Lotion can help to keep your skin soft and moist and prevent itching due to dry skin.
Bacterial Infection
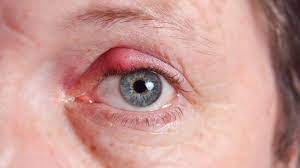 Staphylococcus skin infections are more common and more serious in people with poorly controlled diabetes. When hair follicles are irritated, these bacteria can cause boils or an inflamed bump. Other infections include:
Staphylococcus skin infections are more common and more serious in people with poorly controlled diabetes. When hair follicles are irritated, these bacteria can cause boils or an inflamed bump. Other infections include:
- Styes, which are infections of the eyelid glands
- Nail infections
Most bacterial infections need to be treated with antibiotic pills. Talk with your doctor for effective treatment.
Fungal infections
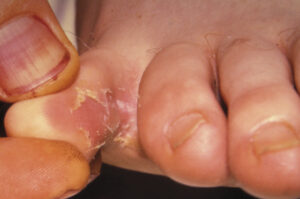
Warm, moist folds of the skin are the perfect breeding ground for these infections.
Three common fungal infections are:
- Jock itch (red, itchy area on the genitals and the inside of the thighs)
- Athlete’s foot (affects the skin between the toes)
- Ringworm (ring-shaped, scaly patches that can itch or blister and appear on the feet, groin, chest, stomach, scalp, or nails).
Different Skin conditions In Diabetes
The skin conditions that diabetes may bring could be-
Acanthosis Nigricans
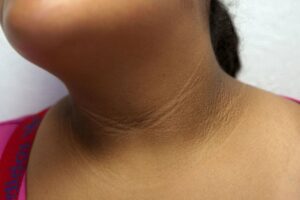
This condition is most common in people with type 2 diabetes. It causes darkened and thickened skin, especially in skin folds. It looks like a small wart. Skin becomes tan or brown. It’s sometimes slightly raised and should look velvety. It is often found on the edges or back of the neck, the armpits, under the breast, and groin. Sometimes, the highest of your knuckles will look strange. This condition usually affects people that are very overweight. It usually starts before diabetes, and it is often a symbol of insulin resistance. While there is no cure, losing weight may help.
Diabetic Dermopathy
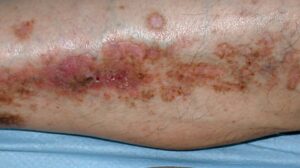
This condition happens thanks to changes to the blood vessels in your skin. Dermopathy appears as a shiny round or oval lesion on the skinny skin of your shins. The patches don’t hurt, and that they rarely cause itching or burning. Treatment usually isn’t necessary.
Necrobiosis Lipoidica Diabeticorum
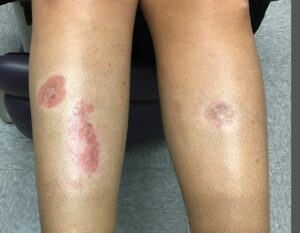
If you’ve had diabetes for an extended time without good control of your blood glucose level, you’ll develop this condition. Poor blood supply to the skin can cause changes within the collagen and fat underneath. The overlying skin becomes thin and red. Most lesions are found on the lower parts of the legs and may become an ulcer if there’s trauma. Lesions have fairly well-defined borders. Sometimes, the condition is itchy and painful. As long because the sores don’t break open, you will not need treatment for them. If the sores do break open, see your doctor.
Digital Sclerosis
Due to poor blood flow, the skin on your toes, fingers, and hands becomes thick, waxy, and tight. It also can make your finger joints stiff. Get your blood sugar under control, because that can help treat this condition. Try lotions and moisturizers to assist soften the skin.
Eruptive Xanthomatosis
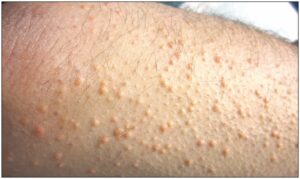
Severe insulin resistance can make it hard for your body to urge obviate fat in your blood. When you have very high cholesterol, this skin condition can happen. Firm, yellow, waxy pea-like bumps on the skin are surrounded by red halos and are itchy. These usually show abreast of the eyes, elbows, face, and buttocks. They can also appear on the rear side of the arms and legs. To treat it, your doctor will work to regulate the extent of fats in your blood. The bumps usually get away over several weeks.
Bullosis Diabeticorum
In rare cases, people with diabetes get blisters that resemble burn blisters. These can affect the fingers, hands, toes, feet, legs, or forearms. They’re usually painless and that they heal on their own. They often happen in people that have severe diabetes and diabetic neuropathy. For treatment, your doctor will assist you to get your blood glucose levels in check.
Disseminated Granuloma Annulare
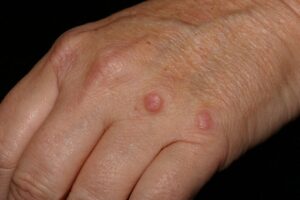
While there’s some controversy over whether this condition is connected to diabetes, this causes sharply defined ring- or arc-shaped areas on the skin. These rashes most frequently happen on the fingers and ears, but they will appear on the chest and abdomen, too. The rash can be red, red-brown, or skin-colored. Treatment usually isn’t needed, but sometimes a steroid medication you set on your skin can help.
Scleredema Diabeticorum
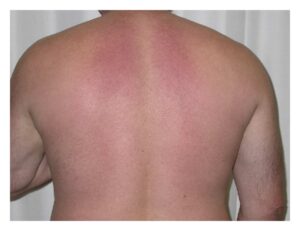
This condition causes a thickening of the skin on the rear of the neck and upper back. It’s rare, but it can affect people with type 2 diabetes. The treatment is to bring your blood glucose levels in check. Lotions and moisturizers might help soften your skin.
After understanding each skin disease or condition that folks with diabetes may experience.
How To Prevent Skin Conditions?
Keeping your diabetes under control is the most important factor in preventing proper skincare and can also help reduce your risk of skin-related problems.
If you’ve got diabetes, there are some steps you’ll fancy to help prevent skin problems.

Tips For Prevention
- Keep your diabetes under control. Follow your healthcare provider’s advice about nutrition, exercise, and drugs. Keep your blood sugar level within the range recommended by your healthcare provider.
- Keep your skin clean and dry. While bathing, use warm water and a moisture-containing soap. After washing, confirm to rinse and dry yourself well (pat your skin dry; don’t rub). Check places where water can collect, like under the arms, under the breasts, between the legs, and between the toes.
- Look at your body after you wash. Make sure you do not have any dry, red, or sore spots that would become infected.
- Avoid bathing in predicament and taking long baths or showers. Also avoid bubble baths, which frequently contain detergents that will be drying. Avoid scratching dry skin. Apply moisturizer instead.
- Keep your skin moist by employing a lotion or cream after you wash. Ask your healthcare provider to suggest a good lotion. Keep a bottle of lotion near the sink so you can use it after washing your hands. You should use a fragrance-free and dye-free moisturizer.
Apply lip balm to prevent chapped lips. - Limit the products you employ on your skin to decrease your chances of getting a reaction.
Treat cuts right away. Wash them with soap and water. Avoid antiseptics, iodine, or alcohol to wash cuts, because they’re too harsh. Ask your healthcare provider to recommend an antibiotic cream or ointment to use on minor cuts. - Drink many fluids, especially water, to stay your skin moist and healthy.
To prevent dry skin when the temperature drops, use an area humidifier to feature moisture to heated, indoor air. - To protect your skin from the sun, use sunscreens with an SPF of 30 or higher on your nose, and wear a hat. In colder months, wear warm gloves and shoes or boots.
Wear all-cotton white underwear. Cotton allows air to move around your body.
Skincare For Conditions Caused By Diabetes

If you have any skin problems, first of all, consult with a doctor. After that you can prepare a first aid kit at home, to make sure that you take care of them whenever needed.
You can keep a first-aid kit handy to take care of your hands and feet. It should contain- antibacterial ointment, gauze pads, hypoallergenic tape or paper tape, and prepackaged cleansing towelettes in case you are out or soap and water are not available.
If you have any blisters, don’t break or pop them. Gently wash the area with a bar of mild soap and warm water and apply an antibacterial ointment. Follow the same process in case of any small cuts, skin irritation, or minor burns. You can also cover them with a gauze pad and secure them with paper tape. If you do so make sure to change the bandage every day.
When To Call The Doctor?
You should call the doctor if you’re feeling itchy anywhere and your condition is not getting any better even after treating the problem. If the pain or discomfort continues for more than two days or you develop a fever. If you notice any pus developing in any part of your body.
Also if you notice any change in your skin, you should mention that to your doctor for sure.
A Word From MantraCare
Do you want to get rid of diabetes? Join our online diabetes consultation program and reverse your Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, dieticians, and health coaches.


