The gmi diabetes treatment is one of the most popular treatments for gmi. It’s also one of the more expensive, but it has many benefits that make it worth the cost. One of these benefits is that gmi diabetes treatment can help you to better control your blood sugar levels. It reduces your risk for complications like amputation, heart attack, or kidney failure.
Another benefit is that gmi diabetes treatment can prevent gmii in adults who are at higher risk for developing type 2 diabetes later on in life.
This means if you have a family history of gmii. Also, other health conditions related to insulin resistance (Metabolic Syndrome) then it might be right for you!
Contents
What is GMI in Diabetes
GMI in diabetes is a proactive, effective way to manage your sugar levels. It offers blood glucose monitoring for people with prediabetes and type-two diabetics who are not on insulin.
GMI takes an active role when it comes to managing the health risks that come along with having diabetes by offering education services about controlling the gmi for diabetes blood sugar levels.
GMI is a proactive, effective way to manage gmi diabetes and keep the risks associated with it at bay.
The GMI can be calculated according to the following formula: GMI (%) = 3.31 + 0.02392 × mean glucose in mg/dL.It was derived by regressing contemporaneously measured HbA1c values against mean sensor glucose levels.
Differences between GMI and A1C
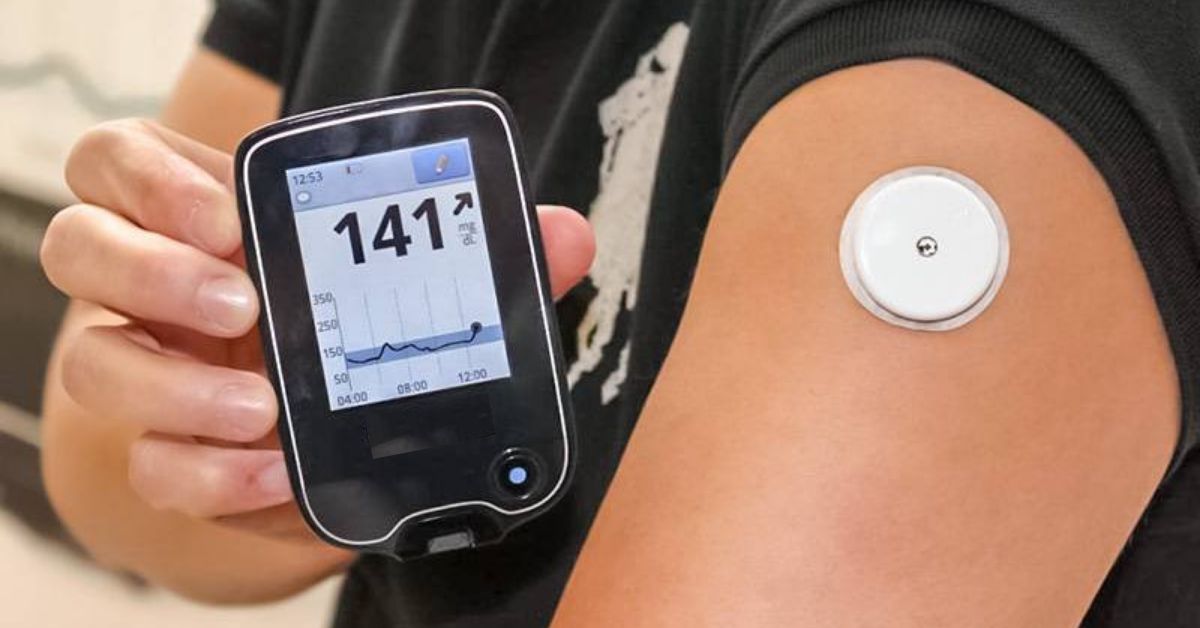
A1C stands for average glucose levels over a two- to three-month period. It is how long it takes for new red blood cells to form. As a result, your A1C level is generally only measured every four months or so. Because the GMI is based on CGM data, you can check it much more frequently than every few months.
GMI measurements are based on CGM data, which can be measured up to every five minutes.
If you have enough glucose readings. Any CGM user can compute their GMI in a matter of seconds. Many CGM devices calculate your average glucose automatically using your mean glucose.
Advantages
To be clear, a GMI can only be calculated if you have a CGM. However, there are still benefits to using GMI if you do have one.
GMI also eliminates misinterpretation of the difference in A1C caused by factors such as kidney disease, iron deficiency, sickle cell disease, the use of specific medicines, and racial and ethnic differences.
With much more variation inside races than between races, two individuals with identical glucose data might have different. A1C levels are based on their rates of red blood cell survival and glucose binding to proteins (often known as glycation). It has a lot greater variation among races.
However, since these same two individuals would have the identical calculated GMI, they would have a more accurate and consistent understanding of their diabetes management and risk of health issues.
The most appealing aspect of GMI (compared to A1C) is that you may (and should) select various timeframes for calculation.
For example, you may compute a GMI for the previous two weeks. You cannot do with an A1C because it measures glucose levels over the preceding two to three months.
Other Advantages of GMI
For many people who have an A1C level at clinical visits two to four times a year. It can be aggravating because it shows a period of high glucose levels rather than the entire diabetes management for that time.
A GMI can be useful in the case of an illness: a clinician or someone with diabetes may select a pre-or post-illness period to evaluate overall glycemic management, including or excluding the time.
Another useful number for determining blood sugar levels during a specific (and even shorter) duration of time is the Time in Range.
It can also be in use to measure the impact of a lifestyle change, such as a new diet or exercise program, or a drug dosage adjustment.
For example, a person could calculate it for two weeks before and after changing their diet to reduce carbohydrates, and then calculate another GMI for the following two weeks.
This may provide a more precise and immediate indication of the impact of the change when compared with an A1C measurement taken at a clinic that cannot focus on the period in question.
A GMI after one to two weeks on a new medication might provide valuable data on whether the dose of the drug should change in addition to tracking daily changes in glucose levels.
GMI and Covid 19
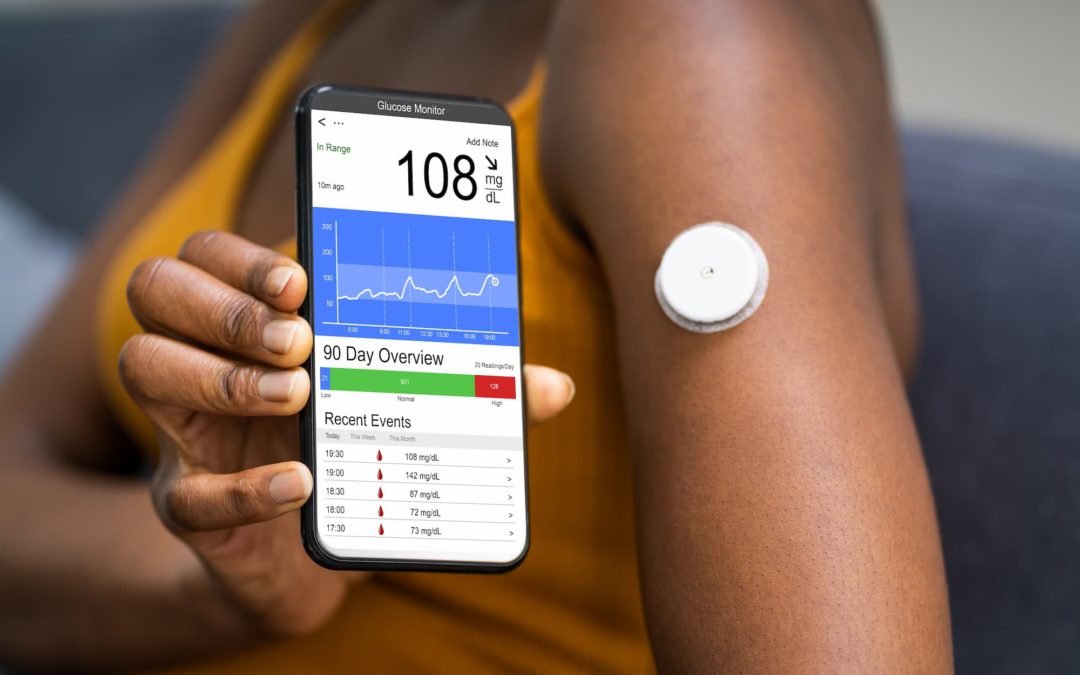
Finally, GMI is a great alternative for a lab-drawn A1C in the era of COVID-19 and enhanced telehealth.
There is no blood draw and no in-person clinic visit required. To be clear, though, keep in mind that your GMI might be higher. It might be lower than your lab-drawn A1C for a variety of reasons mentioned above. It also includes red blood cell turnover, health issues, medications, and more.
The G6PCGMIA can be in interpretation in the same way as an A1C, but because of the variables outlined above, it may also be more precise and serve as a method to evaluate the influence of disease, lifestyle changes, and medication adjustments.
We also aim to assist diabetes management professionals to get more comfortable with GMI and other CGM-derived glucose measurements, which take the whole picture of daily glucose control into account.
A Real-World Analysis
A recent study by the University of Washington compared GMI to real A1C. Even though it is one of the most important CGM parameters and is in use by doctors and diabetics while reviewing glucose readings, there isn’t a lot of information on how it compares to A1C in the actual world.
641 individuals with diabetes were studied at the University of Washington Diabetes Care Center in Seattle, Wash. People had an A1C test conducted within 30 days before or after their healthcare visit when the CGM data was uploaded.
The CGM report had to include at least 14 days of data with at least 95 percent data sufficiency. It means that at least 95 percent of glucose readings were recorded over 24 hours. If a lot of CGM data are missing because the receiver or sensor is too far away or goes more than 24 hours without scanning the sensor, then the sensor is not effective.
Findings
The researchers conducted a study to compare A1C levels to GMI. They discovered that:
- The average difference between A1C and GMI was 0.11 percentage points.
- Only 11% of respondents have less than a 0.1 percentage point difference. This indicates that if their GMI was 7, their A1C was 6.9 to 7.1 percent (or lower).
- According to the CGM, 55% of patients had differences of 0.5 percentage points or less. This indicates that if GMI was 7%, real A1C ranged from 6.5 percent to 7.5%.
- The percentage of individuals with diabetes who had A1C levels above 6.5% was 9.2%. Around one in ten people (9.2%) had an A1C difference of 1 percentage point or more.
- They implied if GMI was 7%, actual A1C was under 6% or over 8%.
The discrepancies surprised the researchers. They had expected larger differences than those seen in prior studies. It sought to discover what might have caused the substantial variances in A1C and GMI.
Conclusion
The use of GMI for Diabetes is a promising treatment. It may be able to help those who suffer from the disease. With no known cure, this new therapy offers hope and relief as it restores insulin production in diabetics. This article has given you an overview of what we know about GMI so far. It also tells how it can work to alleviate some symptoms associated with diabetes.
Do you want to get rid of diabetes? Join our online diabetes consultation program and reverse your Diabetes naturally through lifestyle changes such as a Personalized Diet plan, Exercise, dieticians, and health coaches.


